Chickenpox exposure in pregnancy – avoid rash mistakes
NO
PHARMACEUTICAL INFLUENCE
Chickenpox exposure in pregnancy – avoid rash mistakes
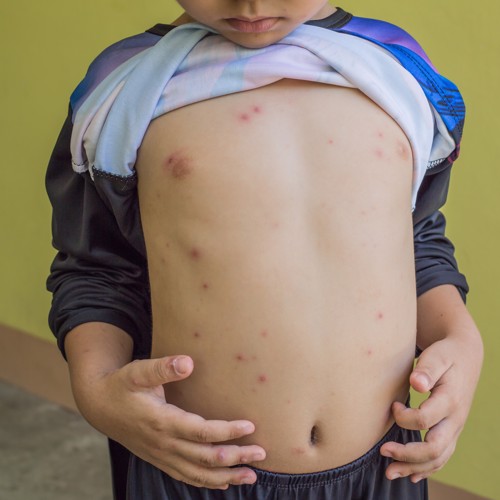
For most of us, when chickenpox strikes, it’s an itchy nuisance for the kids and a childcare headache for the grownups. But for pregnant women, as discussed here, it can result in life-threatening disease, and risks the serious complications of foetal varicella syndrome in the baby as well. Chickenpox exposure in pregnancy is therefore one of those things we want to get right, and new UKHSA guidance from November 2022 and January 2023 takes us through how to do this.
The crucial decision we need to make is whether post-exposure prophylaxis (PEP) is required. This requires us to ask two important questions.
Firstly, is the pregnant woman immune? If she has a history of chickenpox, shingles, or two doses of the varicella vaccine, she can be reassured. If not, she needs a varicella IgG blood test. If the level is <100mIU/ml, unfortunately, she’s not immune.
After this, you need to ask a second question, was the exposure she had significant? The answer to this depends on three things.
- The type of infection in the ‘index’ case she’s been in contact with – contact with chickenpox, exposed shingles lesions, disseminated shingles or an immunosuppressed patient with shingles (who may shed virus in their respiratory secretions), are all considered significant.
- Timing of the exposure –any exposure occurring during the infectious period counts, i.e. from 24 hours before the rash until 5 days after the rash.
- Closeness and duration of contact – household contacts, spending >15 mins in the same room, or a face-to-face contact (such as a conversation) are all important.
Presuming your pregnant patient isn’t immune and has had significant exposure, you’ll need to arrange PEP and that’s where, thankfully, things are finally a bit easier.
Oral acyclovir is now the first choice PEP for women exposed to varicella in any stage of pregnancy. It’s been shown to be as good at preventing chickenpox infection as our previous go-to, varicella zoster immunoglobulin (VZIG). It’s also better tolerated, negates the need for a trip to the big shiny hospital building and is generally preferred by women (no whacking great IM needle for a start). And as those of us who’ve tried (and struggled) to arrange VZIG treatment know, it’s also a lot more straightforward.
When giving PEP, the antivirals should be given from day 7 after the exposure. Research shows this 7-day delay reduces both the likelihood of developing disease, and the severity of it if you do. This is an off-license but well-established use of aciclovir, and we have extensive evidence of its safety in pregnancy
The only reason we would now use VZIG is for a woman unable to take antivirals due to renal impairment, intestinal malabsorption or hyperemesis.
It’s always nice when a guideline makes our lives just a little bit easier, and this one certainly does. The Hot Topics Urgent Care Course will also make your life that little bit easier, covering not just chickenpox in pregnancy but many other urgent care gems. We hope you can join us soon, we’re all ‘itching’ to see you…
Dr Rachel Brettell
16th March 2023
Join us at one of our upcoming courses or live webinars

Recent NB Blogs
Need an immediate update? – all our courses are available on demand
Did you find this useful?
You can quickly add CPD to your account by writing a reflective note about the Chickenpox exposure in pregnancy – avoid rash mistakes post you've read.
Log in to your NB Dashboard and use the 'Add Reflective Note' button at the bottom of a blog entry to add your note.

